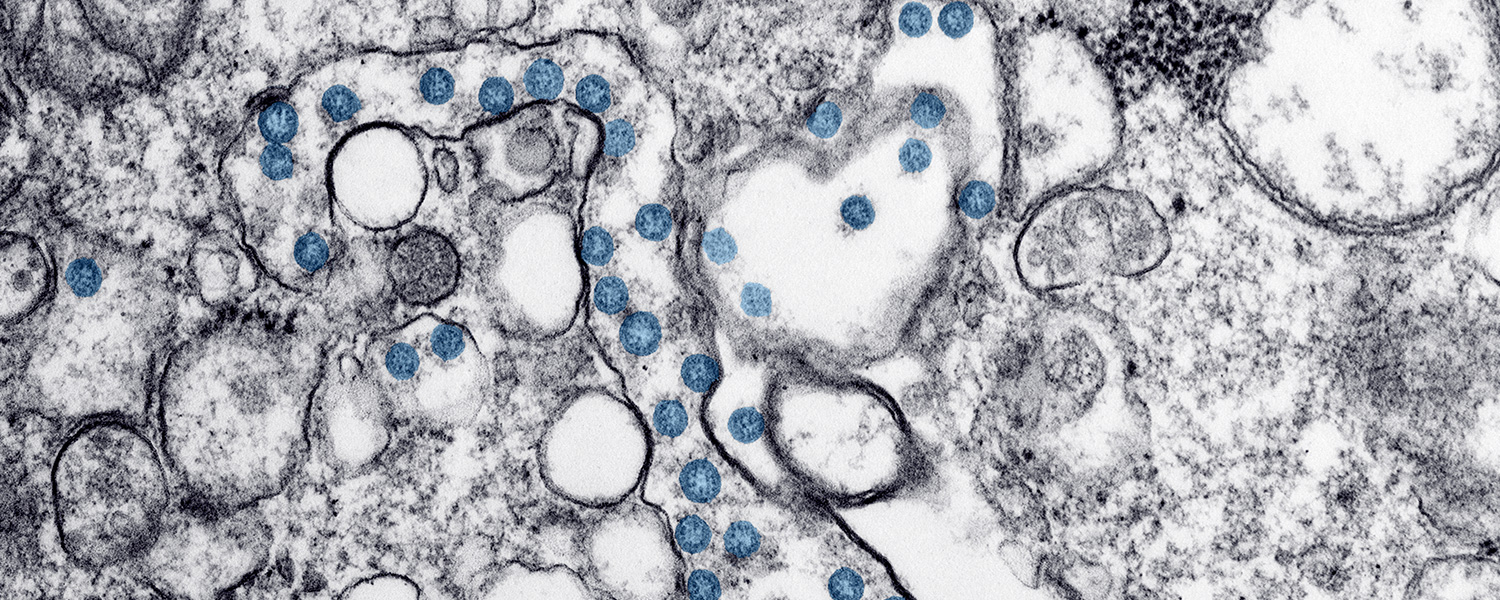
Coronavirus Sleuth
When Triangle universities began to move operations off campus in March, the lab of microbiologist Ralph Baric at UNC-Chapel Hill’s Gillings School of Public Health was ramping up its research on the very virus that was closing down other university research labs.

Baric, who earned both his B.S. in zoology and a Ph.D. in microbiology at NC State, has studied coronaviruses for 36 years. His research lab at UNC, where he is Kenan Distinguished Professor of Epidemiology, is at the forefront of searching for treatments and vaccines for COVID-19, the disease caused by the novel coronavirus.
The coronavirus, officially named SARS-CoV-2, emerged in China back in early December, and Baric first heard about it in early January. Within three weeks, he knew the virus posed a major threat to global health.
“The Chinese reported that the disease resulted from asymptomatic spread and community spread, and was highly infectious. That told me this would be a big problem,” Baric said.
When Chinese scientists reached out to inquire about using an experimental coronavirus therapy that Baric’s lab was developing with Gilead Sciences, he knew the situation was serious. By early March, the U.S. was beginning to see its first cases, and within weeks, much of the country was under stay-at-home orders. That’s when Baric’s lab shifted into overdrive.

Fortunately, his time at NC State prepared him to work hard and excel. Baric was a member of the men’s swimming and diving team, where he earned seven ACC championships and set five ACC swim records. After earning his bachelor’s degree in 1977, he began his Ph.D. program, where he worked with Robert Johnston. He studied alphavirus evolution, replication and pathogenesis, and he developed recombinant DNA techniques for studying viruses.
“I am very glad and proud to be an NC State graduate. My time at NC State was among the best and most rewarding experiences of my life,” he said. “Athletics provided structure, discipline, focus and time-management skills, in the context of competition and camaraderie, the perfect higher education environment for learning new ideas, concepts and skills.”
After completing his Ph.D. in 1982, Baric accepted a postdoctoral research position at the University of Southern California School of Medicine, where he became interested in how coronaviruses replicated, particularly the mouse hepatitis virus strain that was the model virus of the family. “It looked like these viruses had an interesting replication process. So I studied how the viruses replicated and then how they caused disease,” he said.
My time at NC State was among the best and most rewarding experiences of my life.
At UNC, he began to study how coronaviruses jumped between species, and he became convinced that these viruses were high-threat emerging pathogens.
SARS-CoV-2 – which causes COVID-19, an often fatal lung disease – is one of three known coronaviruses that have emerged to attack humans this century. The first was SARS-CoV (Severe Acute Respiratory Syndrome or SARS), a close relative which emerged in 2002 to infect 8,000 people and cause 800 deaths. The second, MERS-CoV (Middle East Respiratory Syndrome Coronavirus), occurred in 2013 and produced a mortality rate of 35%. With both of these diseases, people didn’t transmit the disease to others until they were ill and showing symptoms.
SARS-CoV-2 is different. It is such a successful virus because it is efficiently transmitted by people who have no symptoms. That makes it easy for the virus to spread to a large number of other people. In fact, many people infected with the virus can be asymptomatic or have only mild symptoms, while others become gravely ill.
“Historically, coronaviruses have emerged from bats or rodents through chance encounters with humans,” Baric said. “However, many bat coronaviruses are poised to replicate efficiently in humans, and emerge because human contact is now much more frequent due to greater population density,” he said. “With near-instantaneous global travel, a person can go from the wildest regions in the world to New York City in less than 24 hours, leading to rapid global transmission.”
Baric’s lab is on the front line of studying both treatments and searching for a vaccine for COVID-19. One drug treatment the team is investigating – remdesivir — has been approved for emergency use by the U.S. Food and Drug Administration. Studies showed that it reduced the number of days in hospital for the most seriously ill patients.
Another drug therapy, EIDD-2801, is taken orally and has also shown promise as a treatment that could be used by patients who are not hospitalized. If effective, it could be used as a treatment for emerging coronaviruses in the future.
Baric’s lab is also involved in a UNC System study to evaluate the use of blood plasma from recovered COVID-19 patients to treat others. The treatment has been effective in some COVID patients.
Baric sees reason to hope that worldwide efforts to develop a vaccine will pay off soon. “One of the positive things is the federal funding of the National Institutes for Health has developed new vaccine platforms for emerging diseases,” Baric said. In June, he was optimistic that we could see a vaccine available in 2021.
Working in a lab with a highly infectious virus might seem risky, but not for Baric’s team. “A lot of our people probably think the lab is the safest place to be right now,” he said. With protections like negative airflow into the lab, virus-free air provided in protective hoods, and Tyvek suits worn by researchers, “you are probably as safe as you could be,” he said. “And we have double and triple backup systems.”
Although other university research came to a halt in March, little changed for Baric’s lab. Team members working on other projects were redirected to the critical coronavirus research. Research has been nonstop.
With near-instantaneous global travel, a person can go from the wildest regions in the world to New York City in less than 24 hours, leading to rapid global transmission.
Baric is also a big advocate of wearing face masks to prevent the spread of COVID-19, a measure required of everyone on NC State’s campus. He said masks not only prevent the spread of droplets that can transmit the disease; they also prevent people from touching their faces after contact with the virus on surfaces or receiving aerosolized virus from others.
“In the nations that have controlled the virus, they all wear masks,” he said.
“In early July, after a few weeks of reopening in Phase 2, North Carolina was among the states seeing an increase in COVID cases. While countries like China and Italy saw their high case rates decline, cases in many parts of the U.S. are rising,” Baric said.
It is possible to take steps to reduce the number of cases, he said, pointing out that New York City did it with strict stay-at-home orders, shutting down businesses and transportation, requiring physical distancing and the use of face masks. “Unfortunately, some states aren’t ready to take the disease seriously and implement the right measures to control it,” he said.
“North Carolina has done a pretty good job of controlling the virus,” he said, adding, “but as we open up, we’ll see increased cases if we aren’t very careful. At the moment, the general public needs to take this virus very seriously. It’s a beast that has infected over 38 million and caused over 1 million deaths [as of Oct. 14] worldwide, and it’s not going away any time soon.”
And around the world, people are counting on labs like Baric’s for effective treatments and a vaccine that will allow us return to a more normal lifestyle.
Learn more about doctoral programs in microbiology








Congratulations – Ralph. Well done. Congratulations to NC State too for a great article. Baric Lab – keep up the great work. Great to see a NC State Microbiology alum in the news!!
The first time I’ve seen furin mentioned as related to COVID-19.
This names several antiviral medicine candidates.
Article: An overview of COVID-19 with an emphasis on computational approach for its preventive intervention
https://link.springer.com/article/10.1007/s13205-020-02425-9?utm_campaign=SRBM_AWA_YM01_GL_13205_HP_TrendMDQ420
https://rdcu.be/b8MSl
From an NCSU graduate